Called ex vivo organ perfusion, the technique, device and unique solution were all developed at UHN by a team led by Dr. Markus Selzner, a transplant surgeon and scientist at Toronto General Hospital Research Institute, in collaboration with fellow transplant surgeons at UHN and SickKids. This procedure was part of a clinical trial to assess the safety of the technique, with subsequent studies planned to examine its efficacy.
Zhao Xiao, 53, received the deceased donor kidney which was placed on the device for 3.5 hours, at body temperature. He was able to get up and walk two days after his transplant.
“I feel great,” said Xiao, through an interpreter. “If this can make a difference to other patients, I am glad to be the first one helping them with my experience.”
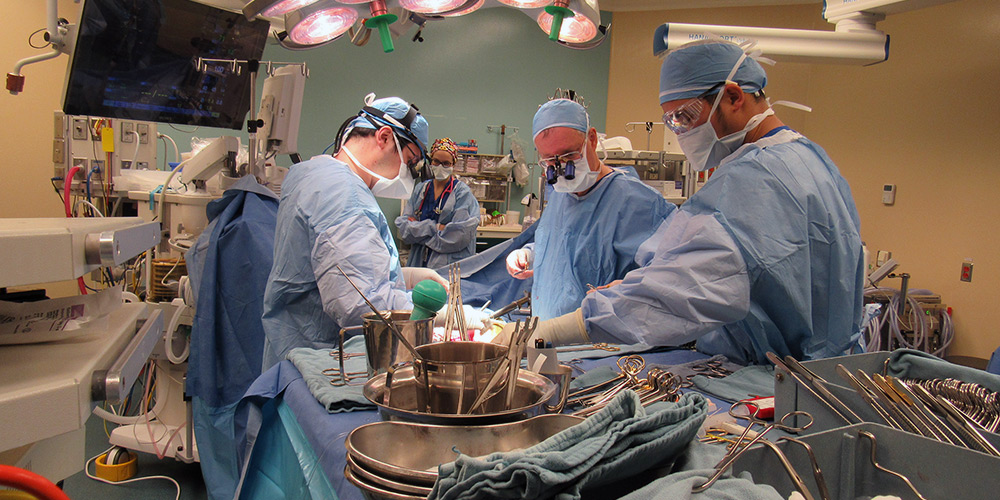
The surgical team performing the first-of-its-kind procedure. (Photo: University Health Network)
Addressing wait times for kidney transplant
Kidneys are the most frequently transplanted solid organ, but a continuing shortage of donor kidneys impacts wait times and quality of life of those waiting for a transplant. Additionally, kidneys are particularly sensitive to traditional “cold storage” organ preservation. The ex vivo organ perfusion technique avoids the damage caused by cold storage and instead allows the donor organ to improve and repair itself, potentially leading to better outcomes for patients.
In the future, ex vivo perfusion may help to increase the number of kidney transplants that can be performed and improve health outcomes for patients. “This technique will allow us to better assess and regenerate the donor organ on the device before we transplant it into a patient, says Dr. Selzner. “We will know how healthy that organ is before the transplant operation.”
Other collaborators on the research and clinical trial at UHN include: Dr. David Grant, Surgical Director of the Transplant Program; Drs. Joseph Kim and Anand Ghanekar, co-leads of the Kidney Transplant Program at UHN; and transplant nephrologist Dr. Istvan Mucsi.
The technique of warm organ perfusion outside the body was pioneered by the Toronto Lung Transplant Program at UHN in 2008 by Drs. Shaf Keshavjee and Marcelo Cypel – again, with support from philanthropic donations. Since 2012, there has been an unprecedented 63% increase in lung transplants at UHN as a result of this system.
